Clearing Aged Non-Replicating Cells Alleviates Cognitive Impairment in Mice
A drug cocktail reduces brain inflammation and improves cognitive function in aged mice
Highlights
· Brain inflammation contributes to brain aging and cognitive impairment.
· Limiting brain inflammation by eliminating aged, non-replicating cells alleviates age-associated cognitive impairment in mice.
Senescence, the phenomenon of when cells get locked into irreversible replication arrest, plays a key role in aging. Clearance of senescent cells has been shown to improve brain function in mouse models of age-related neurodegenerative diseases like Alzheimer’s and Parkinson’s disease. But it is still unknown whether senescent cell clearance alleviates cognitive dysfunction during the aging process.
In a paper published in Aging Cell, Ogrodnik and colleagues from the Mayo Clinic eliminated brain immune cells called microglia that were senescent with senolytics — drugs that target senescent cells for elimination — to significantly improve cognitive function in aged mice. When treated with the senolytic cocktail Dasatinib and Quercetin, aged mice demonstrated decreased activation of brain-specific immune cells called microglia and reduced a milieu of pro-inflammatory molecules known as the SASP (senescence-associated secretory phenotype) that contribute to aging and age-related disease.
“Our data provide proof‐of‐concept for senolytic interventions’ being a potential therapeutic avenue for alleviating age‐associated cognitive impairment,” concluded Ogrodnik and colleagues.
SASP is tied to our last gasp
Senescent cells have been shown to accumulate in a variety of tissues with aging and at the sites of chronic diseases. These cell-cycle arrested cells are thought to exert their detrimental effects with aging and in age-related diseases partially through the SASP. Although the SASP can have beneficial effects, such as orchestrating the clearance of senescent cells, chronic exposure to the SASP is thought to contribute to the spreading of senescence to otherwise healthy tissues.
The aging process is characterized by a progressive decline in memory, attentional control, orientation, and cognition, and aging is a major risk factor for the development of several neurodegenerative disorders. Age-associated cognitive impairment has been attributed to multiple molecular processes including chronic inflammation. But it is not known if the presence of senescent cells and the SASP influences the progression of brain aging and age-associated cognitive impairment.
Senescent cells accumulate in the brain during aging
Ogrodink and colleagues looked into whether senescence impacts cognitive impairment during the aging process. First, they characterized the aging rodent brain at the level of individual cells and found that there was an increase in senescent markers in the brain region associated with learning and memory called the hippocampus in various cell populations. These markers of senescence were more abundant in brain immune cells called microglia.
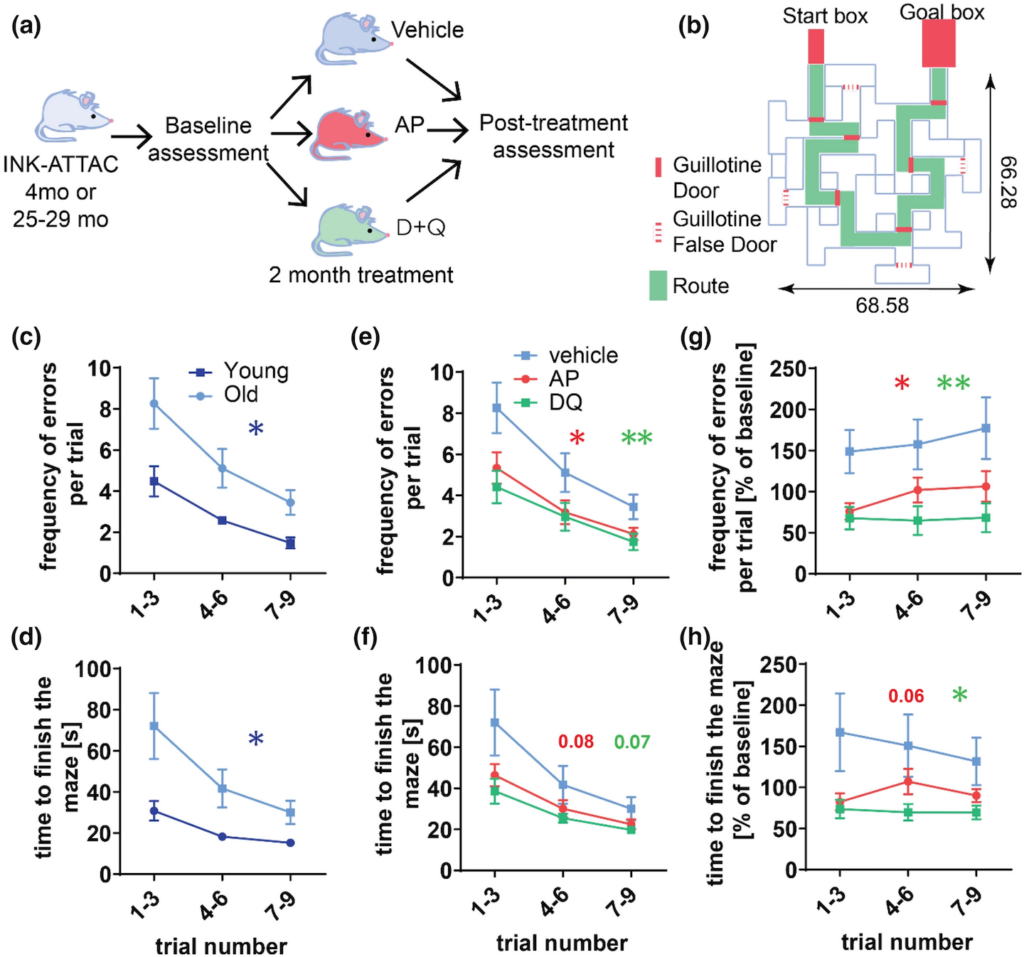
The research team based out of the Mayo Clinic next utilized two models to test how the elimination of senescent cells in the brain of aged mice (25 to 29 months) affected cognitive performance. One model was based on mice that when exposed to a particular drug called AP20187 induce the death of cells positive for a specific senescent marker. The second model was based on treating aged mice with senolytic compounds Dasatinib and Quercetin. These models were then compared to untreated mice of the same age group as well as young mice (4 months).
Perhaps unsurprisingly, untreated old mice had much worse cognitive performance scores compared to the younger mice as measured by a battery of learning and memory tests. But when Ogrodnik and colleagues treated aged mice for two-months with a pharmaceutical agent called AP20187 or the senolytic cocktail of Dasatinib and Quercetin, there was a significant attenuation of age-associated rodent cognitive dysfunction almost to levels seen in young mice. These observations corresponded with a reduction of senescent cells exclusively in the microglial population in the hippocampus.
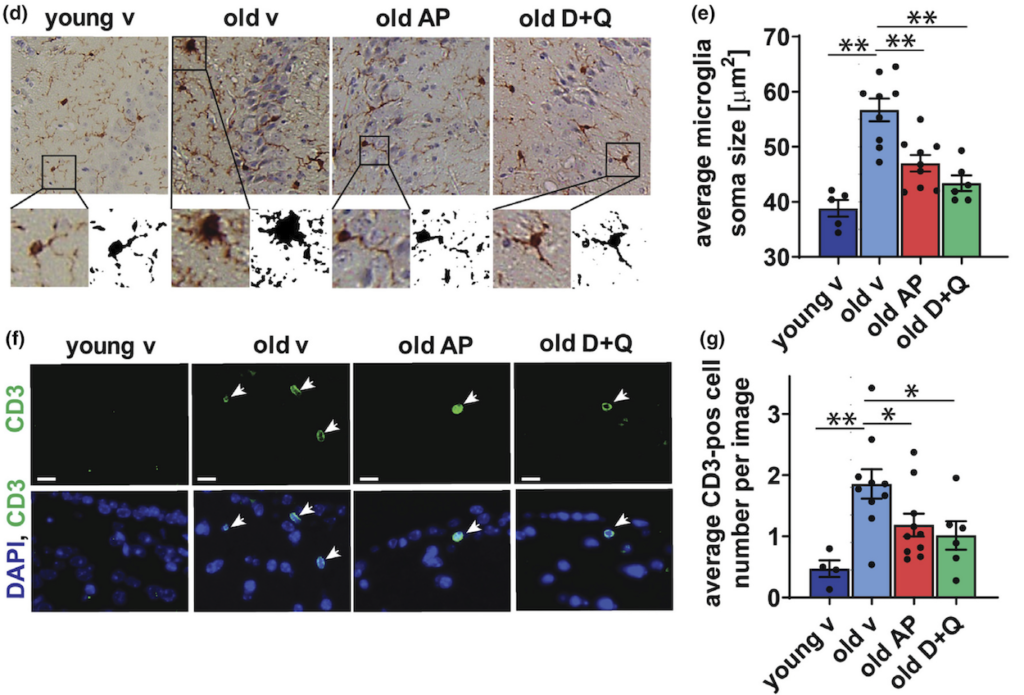
Finally, the Mayo Clinic researchers detected a mild but significant decrease in markers of inflammation, such as expression of pro-inflammatory molecules and infiltration of specific immune cells called CD3+ T cells. Another feature of brain inflammation is microglial activation, which is characterized by increased soma size and is observed during aging and neurodegenerative diseases. Ogrodnik and colleagues found that microglia in the hippocampi of aged mice have significantly increased sizes of soma compared to their young counterparts and sizes of soma are significantly reduced by both treatments.
Together, these data suggest that clearance of senescent cells is a viable therapeutic strategy to counteract age‐related cognitive decline. “On the basis of our findings, we speculate that cellular senescence contributes to the process of brain aging and to driving age‐related cognitive impairment,” proposed Ogrodnik and colleagues. “Our study provides proof‐of‐concept evidence indicating that senotherapies can be tested as a therapeutic approach for rejuvenating the brain and improving memory function in older people.”

