NMN Protects Against DNA Damage-Related Kidney Scarring
Boosting NAD+ after injury suppresses tissue damage and scarring.
Highlights
· NMN improves cell viability after chemical and oxygen deprivation-induced kidney cell damage.
· The NAD+ booster also alleviates kidney tissue scarring from reduced blood flow in mice.
Our kidneys, the organs that keep our blood clean and filtered, can be harmed in all sorts of ways. One major kidney injury results from exposure to toxic chemicals or an inhibited blood supply, which is common in hospitals and affects roughly 25 to 45% of patients in trauma or intensive care units. But, we currently don’t have any therapeutic options to promote kidney tissue repair or prevent the onset of subsequent scarring, or what is referred to as fibrosis in the medical field. For these reasons, there is a need to better understand the progression of kidney injury-induced conditions like fibrosis to generate innovative therapeutic options.
Yang and colleagues from the Peking University First Hospital in Beijing, China published a study in Frontiers in Physiology that identified the molecule nicotinamide mononucleotide (NMN) as a therapeutic option to alleviate kidney tissue scarring following injury. In their publication, they show that NMN inhibits kidney cell damage, aging, and inflammation to prevent and treat tissue scarring. The Beijing-based research team looked at NMN’s therapeutic benefits since previous research indicates that using it helps with DNA damage repair and scarring in other organs. The study suggests that NMN could be an effective strategy to prevent and treat kidney scarring after injury.
NMN the NAD+ Booster
NMN is a precursor molecule to nicotinamide adenine dinucleotide (NAD+), a metabolite in all living cells. NAD+ is critical for fundamental biological processes, namely, DNA repair and energy metabolism, vital processes for cell function and tissue health. Since kidney cells are highly metabolically active, they are very sensitive to NAD+ depletion and impairment of ATP production.
Replenishment of NAD+ levels via administration of its precursors like NMN has been demonstrated to display beneficial effects against fibrosis and age-related diseases. So, it’s possible that by protecting against DNA damage and metabolic dysfunction, NMN may have potential in ameliorating kidney fibrosis.
Boosting NAD+ Preserves Kidney Cells Under Stress
To test NMN’s effects on kidney scarring, Yang and colleagues tested the effects of NMN on cultured kidney cells. Specifically, they looked at whether treating damaged human kidney cells with dissolved NMN could reduce DNA damage senescence, a program that shuts down cell proliferation that is linked to aging.
To do so, they induced kidney cell damage with chemical hydrogen peroxide and also oxygen deficiency, or what’s called ischemia, and then treated these cells with NMN (1 mM). The Beijing-based researchers found that NMN increases cell viability and also decreased the abundance of aged, non-proliferating cells. On top of that, NMN slowed down DNA damage processes in damaged kidney cells that became senescent, markedly diminishing the percentage of DNA-damaged cells from 32% to 22.6%. These findings support that, at least in kidney cells, NMN prevents cell programs that lead to tissue scarring processes.
To see if the protective effects of NMN translated from cultured cells to live animals, Yang and colleagues tested whether NMN treatment impedes kidney scarring progression after induced fibrosis in mice. Since advanced tissue scarring starts with DNA damage and cellular senescence, they first looked at whether treating with NMN diminished DNA damage in mice with kidney damage induced by ischemia and subsequent fibrosis scarring. These mice had elevated DNA damage, however, NMN treatment significantly reduced the DNA damage progression, suggesting that NMN impedes the onset of tissue fibrosis. Yang and colleagues also saw that the kidney damage from ischemia did in fact trigger cellular aging processes that in turn led to cell death and tissue scarring. NMN treatment restored mouse kidney tissue scarring and diminished cell death.
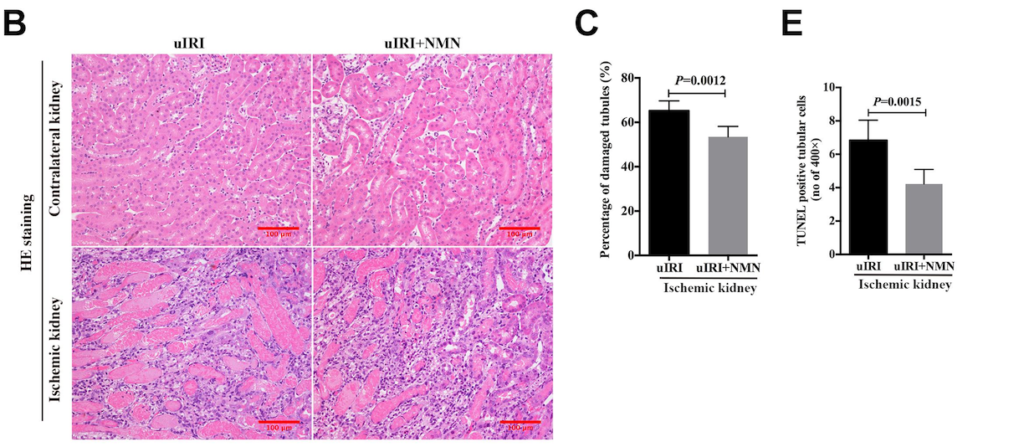
“We observed that stress-induced renal tubular DNA damage occurred upon acute insult and was sustained when subsequent chronic changes (senescence and fibrosis) occurred,” said Yang and colleagues in their publication. “And NMN administration both [live animals] and [cultured cells] showed reduced DNA damage [characteristics].”
These findings provide some support that increasing NAD+ levels with NMN improves DNA repair in kidney scarring, but a direct link between the DNA repair improving tissue scarring requires further study.
Using NMN to Treat Kidney Tissue Scarring
“Collectively, our results suggest the DNA damage inhibition, antiaging and anti-inflammatory effects of NMN in kidneys, and NMN administration might be an effective strategy for preventing or treating kidney fibrosis after [acute kidney injury],” said Yang and colleagues.
Looking into the future use of NMN in injury-induced tissue scarring will require testing if these results translate into people using clinical trials.

