Scientists Reverse Age-Related Infertility by Boosting Mitochondrial Function
Scar tissue accumulation (fibrosis) in ovaries inhibits ovulation — the release of eggs (oocytes) into the uterus — in obese and aged female mice, but removing fibrotic tissue with pharmaceuticals restores oocyte release.
Highlights
- Fibrotic tissue builds up in the ovaries of aged and obese female mice long before menopause, which correlates with declining fertility.
- In obese mice, treatment with pharmaceuticals that improve mitochondrial function and reduce fibrosis restores ovulation and fertility.
- Reducing fibrosis with pharmaceuticals also restores ovulation in aged mice.
With age comes declining fertility for women, typically arising in their mid-30s, sometimes alongside obesity. Even though healthy oocytes persist in most women through their late 40s, researchers have wondered what cellular underpinnings could lead to declining ovulation, the most common cause of infertility. Furthermore, whether similar processes impede ovulation in aged and obese women has remained unclear. By identifying these processes, it’s possible that the age-related decline in fertility could be delayed.
Published in Science Advances, Robker and colleagues from the University of Adelaide in Australia show that the progressive ovarian fibrosis that occurs with age and obesity inhibits the release of oocytes in mice. Amazingly, by treating aged mice with the anti-fibrosis pharmaceutical pirfenidone and the mitochondria-boosting agent BGP-15, which also leads to reduced fibrosis, the Australian researchers restored this ovulation. Similarly, pirfenidone and BGP-15 diminished the accumulation of fibrotic ovarian tissue and restored the number of oocytes released in obese mice. The mitochondria-boosting pharmaceuticals metformin and mitoQ also reduced fibrosis and restored the number of oocytes released in obese mice. These findings indicate that by restoring mitochondrial function and attenuating ovarian fibrosis, fertility can be restored in aged and obese female mice.
Anti-Fibrosis Pharmaceuticals Restore Ovulation
Because studies have shown an overabundance of fibrotic tissue in the ovaries of females that do not ovulate, Robker and colleagues tested whether the short-term usage of the anti-fibrosis agent pirfenidone could restore ovulation in aged female mice. They found that pirfenidone treatment restored ovulation in 60% of aged females. Prior to administering pirfenidone, none of these females were capable of ovulating. What’s more, pirfenidone more than halved the abundance of ovarian fibrotic tissue.
Since mitochondrial dysfunction is linked to fibrotic tissue buildup, Robker and colleagues treated aged mice with the mitochondrial function-boosting compound BGP-15. Like pirfenidone, BGP-15 treatment restored ovulation in aged mice while reducing ovarian fibrosis, indicating that restoring mitochondrial function reduces fibrosis and restores age-related ovulatory decline.
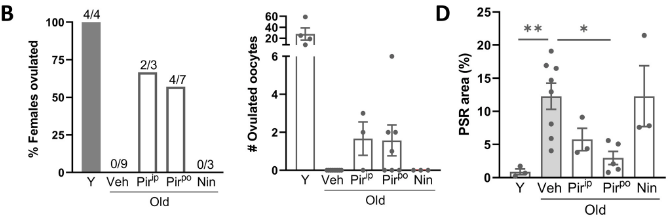
Mitochondria Boosting and Anti-Fibrosis Drugs Restore Fertility
Similar to aged females, Robker and colleagues found that pirfenidone and BGP-15 treatment reduced fibrosis and increased ovulation, as measured by the number of released oocytes, in obese females. Increased oocyte release indicates higher fertility, because although obese females ovulate, the number of oocytes they secrete diminishes. Thus, by reducing ovarian fibrosis with pirfenidone or BGP-15 fertility is restored in obese female mice.
Since the mitochondrial function-boosting compounds metformin and mitoQ can be taken for longer durations than pirfenidone and BGP-15, Robker and colleagues examined whether these agents confer the same benefits. By treating obese mice with either of these pharmaceuticals, the research team found dramatically reduced ovarian fibrosis and double the quantity of oocytes released. These findings suggest that enhancing mitochondrial function and reducing fibrosis with either metformin or the supplement mitoQ can enhance fertility in obese female mice.
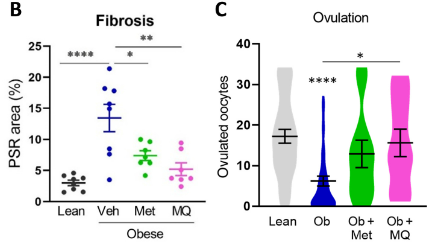
To find how BGP-15 reduces fibrosis, Robker and colleagues analyzed the gene activity and protein abundance of fibrotic tissue. The team found that while BGP-15 did not suppress the gene activation and protein abundance of collagen, one of the proteins that make up fibrotic tissue, it did increase the gene activity of a protein that eliminates collagen, matrix metalloproteinase 13, in obese and aged females. These findings suggest that BGP-15 reduces fibrosis by activating genes that eliminate collagen buildup.
The Study Provides the First Example of Enhancing Fertility with Nonhormonal Pharmaceuticals
“Our findings provide new insight into the mechanism of premature ovarian dysfunction that occurs in premenopausal women and with obesity,” said Robker and colleagues. “These processes could be reversed with existing drugs, creating an opportunity to improve fertility and prolong normal ovarian function in women.”
This study provides the first example of treating infertility with non-hormonal pharmaceuticals in aged and obese female mice. Typically, the hormone human chorionic gonadotropin (hCG) is used to enhance fertility, but it induces serious psychiatric side effects like feeling sadness or emptiness. Moreover, hCG has not been shown to restore ovulation in aged females that have stopped releasing oocytes. For these reasons, using nonhormonal pharmaceuticals like pirfenidone, BGP-15, metformin, and mitoQ provides an exciting alternative to not only potentially increase fertility in aged and obese females but to avoid serious side effects.
Pirfenidone is typically used to treat fibrotic lung disease, and it is currently available for about $60 per 100 mg tablet; however, its use is only recommended for the short term. The anti-fibrosis pharmaceutical BGP-15 costs $65 per 5 mg tablet but is not currently available for patients. The average retail price for the mitochondria boosting compound metformin is around $15 per bottle, but it requires a prescription. Therefore, the simplest option among all of the pharmaceuticals listed in the study is mitochondria-enhancing supplement mitoQ that has a cost of $62.95 for a month’s supply.
Model: C57 Mouse
Dosage: 100 mg/kg injection for four days and 500 mg/kg in drinking water for two weeks of pirfenidone
100 mg/kg injection for four days and 100 mg/kg in drinking water for two weeks of BGP-15
2 mg/mL in drinking water of metformin for two weeks
150 µM in drinking water of mitoQ for two weeks

