Scientists Improve Bone Formation Deficiencies in Glucocorticoid-Induced Osteoporosis
Scientists at Nanchang University discovered NMN may be a therapeutic option for glucocorticoid-induced osteoporosis.
Of the major side effects from glucocorticoid-induced osteoporosis, bone fractures are among the most devastating, affecting 30-50% of patients diagnosed with osteoporosis. Clinicians use glucocorticoids, such as dexamethasone and hydrocortisone to treat patients with inflammation, immunological rejection of transplanted tissue, and autoimmune diseases. In glucocorticoid-induced osteoporosis, patients have “porous bone” when viewed under a microscope, which facilitates weak, brittle bone structures.
This past May, scientists at Nanchang University in China published a study in Molecular Medicine Reports that indicated nicotinamide mononucleotide (NMN) administration attenuates the diminished generation of new bone from glucocorticoid-induced osteoporosis. NMN boosts levels of a molecule called nicotinamide adenine dinucleotide (NAD+), an essential molecule for cellular metabolism. Proteins that depend upon NAD+ for their function, called sirtuins, regulate diverse cellular processes. In a previous study, NMN was reported to improve osteogenesis, bone formation, through the regulation of one of these proteins, sirtuin 1 (SIRT1).
NMN Enhances Bone Formation
In the study, researchers at Nanchang University used bone mesenchymal stem cells, which play an important role in bone formation. They treated these stem cells with dexamethasone, a glucocorticoid responsible for glucocorticoid-induced osteoporosis, and found it inhibited stem cell function. Lower levels of molecular markers indicate bone formation decreased with higher concentrations of dexamethasone. Thus, the results of the experiment confirmed that dexamethasone markedly inhibited the bone-forming abilities of these stem cells.
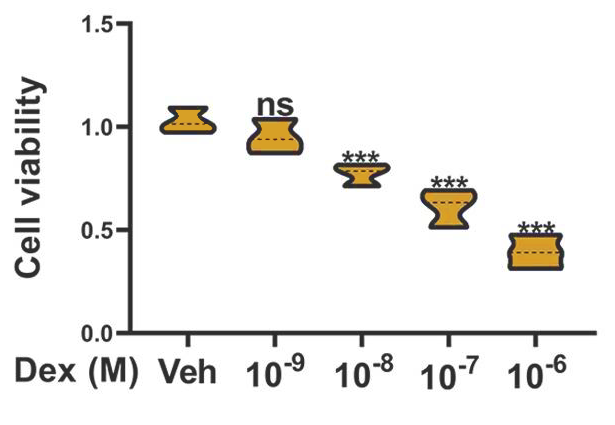
In order to find out whether NMN attenuated the bone formation inhibition of dexamethasone, the scientists applied both NMN and dexamethasone to the stem cells. The expression levels of molecular markers for bone formation increased following NMN treatment. Even though dexamethasone reduced the expression of the molecular markers for bone formation, increasing concentrations of the NMN applied resulted in expression levels of these markers returning to near normal levels.
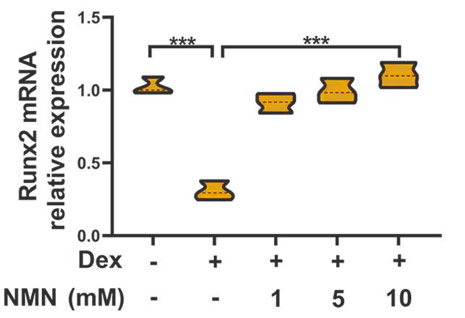 | 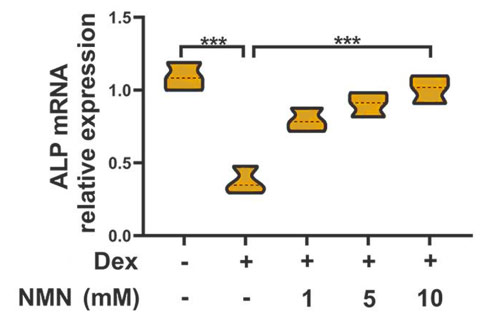 |
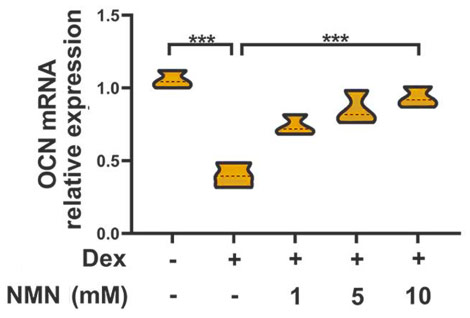
(Huang and Tao, 2020 | Molecular Medicine Reports) Following treatment of bone mesenchymal stem cells with the glucocorticoid, dexamethasone, expression levels of genes involved in bone formation fell. Administering increasing concentrations of NMN following dexamethasone treatment increased the expression levels of these genes.
The researchers then measured the expression levels of SIRT1 to find out whether NMN might enhance bone formation through the activation of this protein. They found NMN did induce higher SIRT1 expression and may promote bone formation in the dexamethasone-treated stem cells. In genetically-modified stem cells with reduced SIRT1 activity, the protective effects of NMN on dexamethasone-treated stem cells were reversed. Results from the genetically-modified cells with reduced SIRT1 expression confirmed the NMN-treated cells with higher SIRT1 expression improved bone formation following dexamethasone treatment.
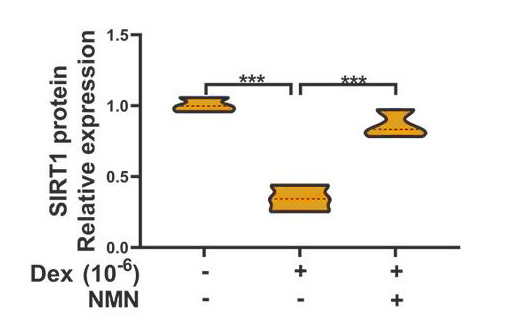
(Huang and Tao, 2020 | Molecular Medicine Reports) Sirtuin 1 protein expression levels significantly dropped following treatment of bone mesenchymal stem cells with dexamethasone, a glucocorticoid. NMN administration significantly improved sirtuin 1 protein expression levels in these cells following dexamethasone treatment.
“The present study suggested NMN as a potential therapeutic target for [dexamethasone]-induced inhibition of osteogenesis, and that [sirtuin 1] was an important downstream target of NMN,” stated the scientists in their study. The expression of molecular markers indicate bone formation decreased following dexamethasone exposure, suggesting this glucocorticoid can inhibit bone formation. NMN attenuated the reduced expression of the molecular markers of bone formation in dexamethasone treatment. The improvements NMN facilitated following dexamethasone treatment were not present in genetically-modified cells with reduced SIRT1 expression, which suggests SIRT1 plays a key role in NMN induced bone formation in glucocorticoid therapy.

