NMN Mitigates the Effects of Age-Related Macular Degeneration
Scientists improve the energy production of cells in the retina, alleviating age-related macular degeneration.
Age-related macular degeneration (AMD) constitutes the leading cause of vision loss in adults and affects 20-30% of people over 75 years of age in developed nations. Individuals with AMD have difficulties reading, recognizing faces, and visualizing fine detail. But current treatments for AMD can only treat about 10% of the patients, those with “wet” AMD, where blood vessels grow into the center of the eye. No treatment options currently exist for the other 90% of patients with “dry” AMD who lose cells in their retina, the light-sensitive tissue of the eye.
As past studies indicate that defects in the mitochondria, the cell’s energy generator, are key aspects of the AMD disease, a new study shows that targeting the organelle can treat dry AMD. The research team from the University of Minnesota Department of Ophthalmology published a study in Redox Biology where they treated mitochondrial dysfunction in cells from AMD patients with four molecules: N-acetyl-L-cysteine (NAC), rapamycin, pyrroloquinoline quinone (PQQ), and nicotinamide mononucleotide (NMN). Cells from different AMD patients exhibited a distinct reaction to each drug suggesting the potential of developing personalized treatments for individuals with AMD. In other words, some treatments work in certain patients and not others so that clinicians could evaluate which treatments are most effective in each individual.
Mitochondrial modulators improve retinal cell energy production
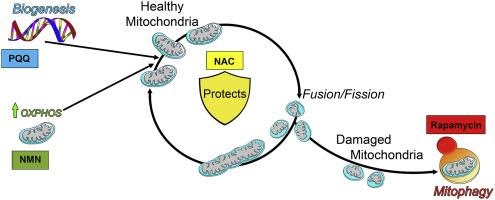
Ebeling and colleagues chose these four molecules based on their effects on mitochondria. NAC increases cellular amounts of energy molecule adenosine triphosphate (ATP) by protecting mitochondria from oxidative stress and thereby increasing the amount of mitochondria that produce ATP. PQQ is can increase mitochondrial content in cells through stimulating mitochondria production. Rapamycin increases the number of mitochondria and induces the disposal of defective mitochondria from the cell, a process called mitophagy. NMN boosts the concentration of a molecule called nicotinamide adenine dinucleotide (NAD+), which promotes cell production of energy and maintenance of health.
By measuring the ATP levels, scientists can evaluate how well mitochondria function. Ebeling and colleagues treated donor eye cells with the four molecules, which only improved mitochondrial function in some of the AMD patients. Of the four molecules, rapamycin, PQQ, and NMN significantly increased ATP levels in patients’ retinal cells, whereas NAC did not.
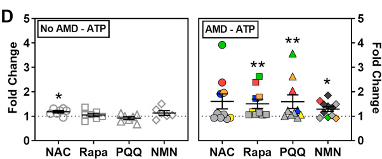
Depending on the patient, the cells exhibited highly individualized responses to these four molecules. The treatment improved mitochondrial function in half of the patients’ retinal cells 50% to 350%, while the other half showed a 5% to 25% improvement in mitochondrial function.
“These results support the idea that an individualized approach to treating AMD is required. Developing ways to pre-screen patients to determine the optimal type of intervention is a critical linchpin in finding effective treatments for AMD,” stated Ebeling and colleagues.
The University of Minnesota found that, out of the four molecules, PQQ was the most effective in improving mitochondrial function. Ebeling and colleagues posit that although variability existed in the treatment responses, a particular cocktail of molecules could lead to better treatment responses.

